
On 10 September, Storm Daniel made landfall in Libya. Pounding rain and 80mph winds battered the eastern shore as the storm destroyed two dams in the port city of Derna. Seven-metre-high waves came crashing into the city as the torrent of water swept entire neighbourhoods into the Mediterranean.
Amidst the mud-soaked remnants of Derna’s worst hit neighbourhoods, the human toll of the disaster was difficult to discern. This is still the case today. Estimates range from 4,000 to more than 11,000 deaths; a figure that may never be verified. According to the search teams that arrived in the aftermath, many victims had been swept out to sea.

Climate Change and Conflict: Precursors for Catastrophe
Storm Daniel was what is informally termed a ‘medicane’; a tropical-like cyclone that forms over the Mediterranean, normally at the end of summer. Excess heat contributes to their formation. In the summer preceding the storm, southern Europe was experiencing a blistering heatwave, and with rising sea temperatures in the Mediterranean, this made a devastating medicane far more likely.
Prior to the flooding, Libya was ill-prepared to deal with a disaster of this scale. Continued political turmoil and two civil wars in little over a decade had left public services – particularly health, social protection, and education – in a fragile state. Eastern Libya was already home to 46,000 internally displaced people before the floods, of whom 2,800 were living in Derna. The flooding more than doubled this number, with more than 50,000 survivors being displaced.
Supporting Local Healthcare in Derna
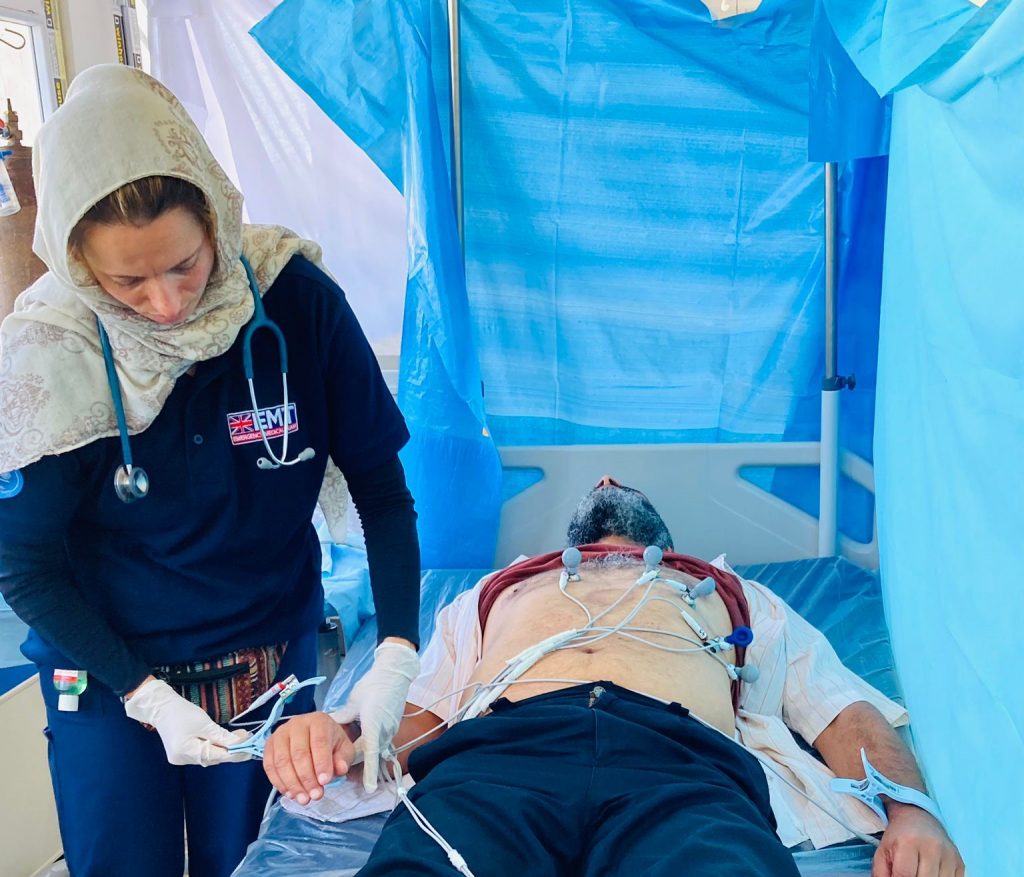
As the UK’s Emergency Medical Team (EMT), our staff deployed to Libya on 27 September and began providing mobile health care one week later in Derna, through direct support to primary health clinics. Our multi-national team comprised of doctors, nurses, pharmacists, and support staff.
We quickly scaled up our response, supporting a maternity unit, providing essential medicines and supplies, and delivering training on a range of topics requested by Libyan colleagues. Working alongside Libyan health workers, local authorities, other international organisations and EMT partners, our team sought to ease the burden on Derna’s already fragile health system and providing much needed respite for local healthcare staff.

“There were clear needs to support the local population with primary health care and mental health and psychosocial support, given that many of the pre-existing primary health clinics had been damaged and many health workers had tragically been killed,” said David Anderson, UK-Med’s Medical Coordinator in Libya.
“What we must all remember is that the local health care staff also lived through this terrible tragedy and lost family and friends and yet somehow found the resolve to continue to support their local communities. Supporting those health workers is a crucial part of any response,” he said.
At the Dar as Salam clinic in Derna, one of our mobile teams treated a mother whose 11-year-old daughter had been killed in the flood. One of her young sons had also been pulled unconscious from the water, but thankfully was still alive.
Their family doctor had been killed in the floods too. The mother’s asthma was worsening, her steroid inhaler was empty, and she was experiencing shortness of breath. But without access to healthcare in the aftermath of the disaster she struggled to access medical care.
The clinical team assessed her condition and provided her with a new inhaler to manage her asthma attacks as well as mental health support, given she had experienced immense grief and anguish at the hands of such a devastating disaster.

“The disastrous floods not only devastated towns in Libya, but also caused huge psychological trauma for many of the survivors,” - Jemma Berwick, UK-Med nurse.
After delivering three-weeks of primary healthcare to flood-affected communities in Derna, the UK-funded emergency medical teams left eastern Libya last week, concluding their in-country presence that was able to bolster local health care facilities to help reach many communities who otherwise had little access to healthcare.
Working with UK-Med
If you have the determination to make a difference, and would like to work with UK-Med, visit our vacancies page or follow us on LinkedIn.
UK-Med staff fall into three main categories: core staff, country programme staff, and register members. Core staff are full-time employees of UK-Med and ensure the continuing function of our operations overseas and at headquarters. Country programme staff are part of our more established and longer-term humanitarian responses, such as our current Ukraine mission. Register members are recruited to support surge and emergency response requirements, volunteering to be on call for certain times of the year. They deploy for short periods at a time (usually between 4-12 weeks).
UK-Med doesn’t only recruit clinicians. We draw on a wide range of specialisms to support our mission, including logistics, operations, human resources, communications, and finance.
We are continuing to strengthen our register of trained humanitarian and health professionals to enable us to respond to emergencies around the globe, and we will be running a campaign for UK based health roles at the end of 2023 and into early 2024. Keep checking our website and LinkedIn page for more details which will be shared soon.






